One Family’s Journey Through Lyme Disease and Their Nontraditional Path to Healing
“Biting Back”
The following story was submitted by an Austin Air customer.
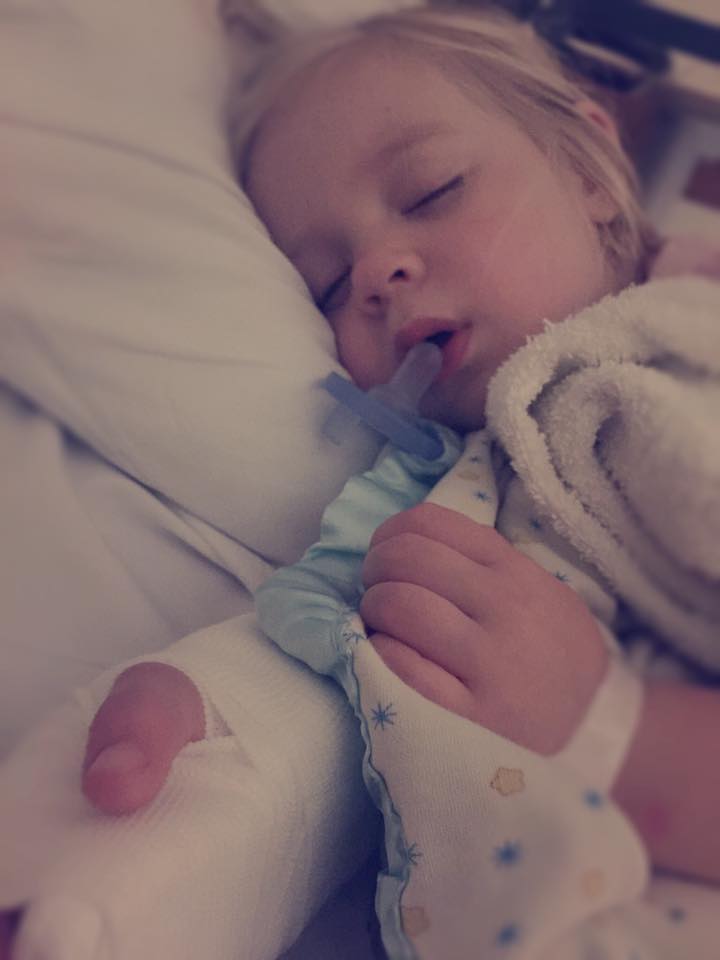
My daughter was three when I saw it. On her lower left abdomen, it resembled a small bubble of dried blood (the size of a chia seed). I assumed it came from a scratch. When I tried to look at it closer, she wiped it away and hurried off to play. All that remained was a small, light-red dot. And so, I thought nothing more of it.
Until exactly five days later.
That tiny red dot became the center of a bullseye rash that covered her entire abdomen. It came ferociously with a fever of 105 degrees, an enlarged spleen, respiratory difficulty, hallucinations, and full-body pain.
The diagnosis: Lyme Disease.
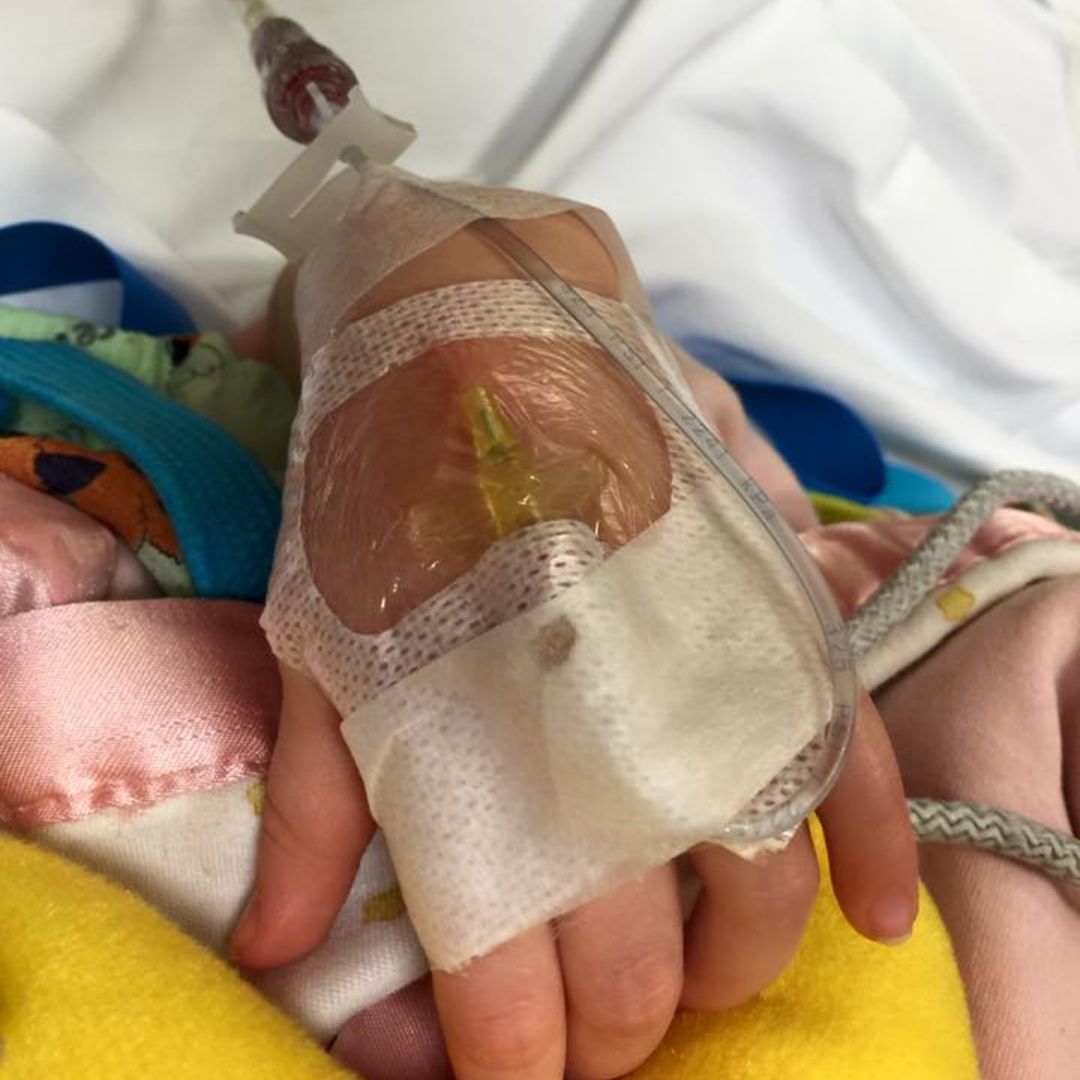
She was released from the hospital with high-dose antibiotics and the hope that our firecracker of a three-year-old would soon be shooting off to play again. But she finished the antibiotics and still wasn’t playing. She still wasn’t walking. She still wasn’t better.
They started her on another round of antibiotics (a different kind). Near the end of that round, she still couldn’t hold a crayon because of arm pain. She still couldn’t walk because of leg pain. She still wouldn’t come out from under a blanket without sunglasses because of light sensitivity. She still had insomnia, shallow breathing, an enlarged abdomen, panic attacks, recurring fevers, full-body spasms, air hunger, and strange intermittent rashes.
We were told it was antibiotic-resistant Lyme disease. We were told there was nothing more they could do for her. We were told to see a Lyme specialist.
Unfortunately, at that time, most Lyme specialists in the United States were not pediatric care providers. Our daughter wasn’t 18, so they couldn’t see her. We tried to schedule her at a nearby children’s hospital, but they were scheduling five months out. Five months.
We were forced to consider alternative (naturopathic and functional medicine) therapies. And I’m glad we did. We dug long and hard for answers. And we finally began to unearth the information needed for healing.

The Inaccuracies of Traditional Lyme Disease Testing
Information regarding Lyme disease was hard to find via traditional means. The reason: Lyme is extremely difficult to diagnose and sometimes even more difficult to treat.
Insurance records suggest that approximately 476,000 Americans are diagnosed and treated for Lyme disease each year. (1) And a 2019 study indicated that more than two million people in the United States may suffer profound disability from post-treatment Lyme disease syndrome (PTLD). (2) These numbers could actually be higher as many people might not know they are infected. Many people never develop the classic bullseye rash. And current testing for Lyme disease is often unhelpful.
The two most common diagnostic tests for Lyme are the enzyme-linked immunosorbent assay (ELISA) and the Western blot. Both test for antibodies that would form in someone infected with Borrelia burgdorferi, the bacteria that causes Lyme disease.
Unfortunately, the ELISA is falsely negative nearly 50% of the time. Sadly, this is where help ends for many Lyme sufferers as some insurance companies will only pay for one test.
Some doctors might continue to look for Lyme disease after a negative ELISA by running a Western blot. This test looks for reactivity against ten different proteins commonly found in the Lyme bacteria. The CDC says five bands must come back positive for a diagnosis.
However, in one study, the CDC’s standard two-tier testing for Lyme disease failed to accurately diagnose more than 70% of blood samples. (3)
Therefore, some practitioners believe that Lyme treatment is warranted if the patient has symptoms of Lyme disease and any of the high-probability bands come back positive (high probability band numbers are 23, 31, 34, 39 or 93).

Lyme Disease Coinfections Are Also Difficult to Diagnose
Now, let’s say you’re one of the “lucky” few (like my daughter) who happens to get a positive diagnosis from the ELISA or Western blot. That’s still only half the battle.
Lyme disease is typically caused by the bacteria Borrelia burgdorferi carried by black-legged, hard body ticks. (Though, the Lyme bacteria has also been found in mosquitoes, fleas, and flies.) (4) In addition to Borrelia, ticks can also carry other bacteria, parasites, and even viruses (sometimes simultaneously) that can cause debilitating coinfections.
According to the research of Graham et al. (2007), those that are coinfected by multiple parasite species seem to be the rule rather than the exception. (5) The most common coinfections appearing with Lyme disease include Babesia, Bartonella, Ehrlichia, Mycoplasma, Rocky Mountain Spotted Fever, Anaplasma, and Tularemia.
These are also hard to diagnose, though.
Babesia organisms, for example, can create immune escape variants in response to vaccinations, forestry changes, and medications. In fact, ranchers will often put antibabesial drugs in the feed of their cattle to prevent infection. But, these types of prevention strategies can give way to drug-resistant parasites. The organisms can become so adaptable that the same species may take on forms (even behaviors) that make them unrecognizable from one host to the next. (6)
What’s more, these organisms can cause severe symptoms but might only be present in 1% of red blood cells (again, making it very difficult to diagnose). For this reason, some practitioners find it helpful to run Polymerase Chain Reaction (PCR) testing in conjunction with a blood smear analysis when looking for coinfections like Babesia. While PCR is not 100% accurate, these tests are increasing their sensitivity to various coinfection species.
Some functional medicine practitioners will also run labs such as TGFb1 and Complement C4a which are often elevated in biotoxin illnesses (whether it’s Lyme, coinfections, or both). However, studies have shown that serum TGFb1 levels may not spike until 56 days post-Lyme infection. So some practitioners may not consider this useful in the beginning stages of the disease. (7)
Some practitioners take a more in-depth look at symptoms through tools such Horowitz Lyme-MSIDS Questionnaire developed by one of the leading authorities on Lyme Disease, Dr. Richard Horowitz. He also authored the book “Why Can’t I Get Better?” which I’ve read, re-read, and read again. It is very highly recommended.

Lyme Disease Supplements for Detoxification and Methylation
With the help of a trained practitioner, we began to explore the possibility that our daughter had various coinfections (given the number of years she had suffered and the symptoms she still experienced regularly).
The most common symptoms of early Lyme disease resemble symptoms of the flu. But infection can then spread to the joints, gastrointestinal tract, lungs, and the heart (Lyme carditis).
If left untreated, tick-borne illnesses can also cross the blood-brain barrier and infect the central nervous system (8), especially in children. This can result in something known as Lyme Brain — sometimes also referred to as Lyme-Induced Leaky Brain or Neuroborreliosis — causing symptoms of anxiety, panic attacks, insomnia, depression, numbness, pain, weakness, facial palsy, visual disturbances, stiff neck, and severe headache.
Sometimes pathogens will leave the blood and actually enter the brain. Immune cells then enter the brain, too, in an attempt to eradicate the pathogen. Sometimes this creates a hyper or autoimmune situation that can result in meningitis (inflammation of the meninges, the outer membrane of the brain, and spinal cord) or encephalitis (inflammation of the brain itself).
To combat the infections running rampant in our daughter, our practitioner guided us toward homeopathic antibacterial therapies (remember, her illness was resistant to traditional medication). Part of the strategy was to support her detoxification pathways, too. That way, the deteriorating pathogens would not accumulate in her body but instead be safely eliminated. We focused especially on her liver and methylation.
Methylation is a bodily process that drives the immune response, controls inflammation, and enables detoxification, among many other things. In order for the body to methylate properly, it needs a healthy supply of folic acid. Unfortunately, our daughter has a genetic MTHFR mutation. That means she can't properly convert folic acid into its usable form (methyl folate). Without enough folate, a person cannot methylate properly. Without proper methylation, one can’t detox well and the immune response is impaired.
And it’s not just our daughter. It has been estimated that 40% of the population could have a genetic MTHFR mutation impairing methylation. (9) Some estimate the number could be as high as 60-70%. (10)
Part of our strategy then was to support our daughter’s methylation by supplementing with bioavailable folic acid, also known as methyl folate. We also used clay minerals to adsorb various endotoxins.


A Lyme Disease Diet to Unburden the Immune System
As I reflect on our daughter’s Lyme journey, it is clear that supporting her immune system was one of the most beneficial things that we did. The Lyme bacteria and its coinfections launch an attack on the immune system. Borrelia even prevents immune cells from “marking” it as a foreign invader, thus giving the bacteria free reign in the body. (11)
For this reason, it is crucial to limit exposure to other toxins – such as those found in processed food and air pollution. Otherwise, these can overburden the immune system, making it very difficult to fight the Lyme bacteria.
To start, we eliminated all foods from her diet that were known to be inflammatory. This included hydrogenated oils, fried foods, soda, gluten, dairy, corn, highly processed boxed or canned foods, and neurotoxins such as MSG, high fructose corn syrup, and food dye.
We also eliminated foods that can have a negative impact on gut health as 80% of immune cells reside in the gut microbiome. (Certain gut microbes even act as the gatekeepers for the inflammatory response.) These included sugar and artificial sweeteners such as aspartame (found in Equal and NutraSweet), sucralose (found in Splenda), and Saccharin (found in Sweet 'N Low).
Instead of these inflammatory foods, we fed our daughter anti-inflammatory whole foods that were closest to their natural form, as they are found in nature. We included lean, organic proteins as well as many fruits and vegetables, especially those high in antioxidants and fiber (which is beneficial for good gut health). We also included garlic, onions, and herbs such as thyme and oregano when she could tolerate them as these contain anti-inflammatory, antibacterial, and antiviral compounds.


Harmful Airborne Pollutants That Weaken the Immune System
While it’s often overlooked, air pollutants can stimulate pro-inflammatory immune responses in the body. It’s not just common allergens that trigger this. And it’s not just in cases of asthma and chronic obstructive pulmonary disease (COPD). Pollutants such as particulate matter, VOCs, and mold can have a severe impact on immune function in anyone–especially those with Lyme Disease.
1.) Particulate Matter
When inhaled, small particulate matter (with a diameter < 2.5 μm) can cross the alveolar-capillary barrier and travel to other organs in the body. Inhaled air pollution can even affect the gastrointestinal tract (12), again, where 80% of the immune system resides.
Indoor particulate matter can be produced by cooking, burning candles, smoking cigarettes, running gas appliances, and using fireplaces, space heaters, or kerosene heaters. It is also produced by motor vehicle traffic, outdoor barbecues, and gasoline-powered lawn and garden equipment that can be brought into the home through open windows and doors.
2.) VOCs
Other airborne pollutants such as some volatile organic compounds (VOCs) can lead to immune system disorders, too. (13) VOCs are gaseous compounds emitted from common household items such as new carpet, new furniture, paint, cleaning supplies, and even some electronics.
3.) Mold
One of the most dangerous airborne pollutants for Lyme sufferers is mold. Why? Because mold can produce toxic chemicals known as mycotoxins, which can travel through the air and be inhaled. These mycotoxins can weaken the body’s ability to fight off infection – putting a person who is already fighting an infection (like Lyme disease) at a greater risk of mold-related illnesses such as Chronic Inflammatory Response Syndrome (CIRS) and Mast Cell Activation Syndrome (MCAS). Not only that, but mold can also affect the nervous system, endocrine system, digestive system, cardiovascular system, and respiratory system.
And it’s even worse for people with (like my daughter).
The Human Leukocyte Antigen (HLA) is a marker that the immune system uses to differentiate which cells belong to the body and which cells are foreign to the body. When an antigen is presented correctly, the immune system properly identifies foreign invaders (such as mycotoxins and Borrelia) and then removes them. But the HLA-DR gene prevents the immune system from properly identifying mycotoxins and Borrelia as invaders. So the immune system doesn’t make the antibodies needed to remove them.
If they’re not removed, these toxins can accumulate in the body. Worse yet, they can be stored in “fatty” areas such as the brain. And because no antibodies are produced, mold and Lyme can go undiagnosed for weeks, years, even a lifetime.
Another important thing to keep in mind regarding mold is that it’s not just inhaled. It can also be eaten. Though it’s not always evident by the fuzzy green stuff you see on aging bread, cheese, or produce. Mold can hide in other seemingly harmless foods, too.
Take coffee, for example. Not only is coffee one of the most chemically-treated foods on the planet, but it’s also known to contain high levels of mold. One study showed that 91.7% of green coffee beans were contaminated with mold. (14) Of all the mycotoxins found in coffee, Ochratoxin A (also known as OTA) has been touted as the most dangerous because it is listed as a possible carcinogen. What’s doubly important for Lyme sufferers is that OTA is also an immunosuppressant, and is especially harmful to the kidneys.
For this reason, it may be beneficial to look for organic coffee beans that are third-party tested and free of mold. My favorite is Cardiology Coffee by Dr. Wolfson (who just so happens to be an Austin Air dealer).


Air Purification: A Crucial Component of Lyme Disease Treatment
To further support our daughter’s immune system, we deployed Austin Air purifiers in her bedroom as well as in other rooms throughout the house. This has proven to be quite beneficial. Her quality of sleep has greatly improved, and so has her anxiety and morning congestion.
The Medical Grade HEPA used in the Austin Air Healthmate Plus® removes up to 99% of bacteria and aerosolized viruses larger than 0.1 microns. It also removes mold spores. The carbon and zeolite blend even takes care of the mycotoxins that can develop when mold is present. The carbon and zeolite blend also eliminates various gases, chemicals, VOCs, and formaldehyde.
Because of this, the Healthmate Plus helps strengthen the immune system and reduces the viral load to lower the risk of infection or severity of disease, making it perfect for individuals like my daughter who are suffering from preexisting conditions and Multiple Chemical Sensitivity (MCS).
Similarly, the Austin Air Bedroom Machine® also uses medical-grade HEPA and activated carbon, but it has an additional layer of protection. It uses a military-grade HEGA carbon cloth to not only capture viruses but deactivate them. The Bedroom Machine was proven in two separate clinical trials to be highly effective at removing dangerous airborne pollutants from the home.


Looking Ahead After Lyme Disease
It’s been more than 5 years since my daughter was first bitten by that chia-seed-looking tick. In that time, we’ve learned more than we really cared to about this insidious disease. We’ve learned about testing, coinfections, homeopathic therapies, gut health, inflammation, detoxification, methylation, genetics, diet, and air pollution (to name just a few).
That’s why we feel obliged to tell our story.
After hearing “there’s nothing more we can do for you,” she’s now making progress. After hearing “there is no cure,” she’s finally starting to heal. My daughter is sleeping through the night (most days), making friends, and even playing sports. She’s eating clean, breathing clean. By golly, our little firecracker is biting back.


References
1. https://www.cdc.gov/lyme/datasurveillance/index.html
4. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3542482/
5. https://www.sciencedirect.com/science/article/abs/pii/S1471492207000876
6. “Natural Treatment for Lyme Coinfections: Anaplasma, Babesia, and Ehrlichia” by Stephen Harrod Buhner; Healing Arts Press Rochester, Vermont; February 1, 2015 ISBN #978-1-62055-258-2
7. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4045338/
8. Raxlen, Bernard, M.D. with Cashel, Allie. Lyme Disease: Medical Myopia and the Hidden Global Pandemic. Hammersmith Health Books: London, 2019 (100)
9. https://www.ahajournals.org/doi/10.1161/circulationaha.114.013311
10. https://www.racgp.org.au/afp/2016/april/mthfr-genetic-testing-controversy-and-clinical-imp
11. https://www.hopkinsmedicine.org/news/newsroom/news-releases/research-story-tip
How to Pay for Your Austin Air Unit Using Your Flexible Spending Account
Learn More

The Hidden Toll of Wildfires: A Crisis Beyond the Flames
Wildfires are among the most dramatic and destructive events of our time—burning homes, displacing communities, and reshaping entire landscapes. But beyond the visible devastation, a quieter and more insidious crisis is unfolding. As the climate warms and wildfires become more frequent, researchers are uncovering new ways these events are threatening human health. We’ve long understood that wildfires destroy property and worsen air quality. But now, studies show they’re also reversing decades of progress under clean air laws, creating widespread exposure...

Feeling Sick: Is It a Summer Cold or Wildfire Smoke?
It’s summer—the season of sunshine, fresh air, and... coughing? Sneezing? A sore throat? If you’re feeling under the weather in June or July, you’re not alone. But is it just a harmless summer cold—or could it be wildfire smoke? With wildfire smoke drifting across the country and summer viruses making the rounds, it’s no wonder so many people are sniffling, coughing, and wondering what’s going on. These two health hazards can cause surprisingly similar symptoms—but they require different responses. Here’s...

Cold and Flu Season Survival Guide for Families
Cold and flu season is a challenging, somewhat miserable time. But it can be especially tough for families with children, elderly relatives, or members with chronic health conditions like asthma or COPD – who are at higher risk of complications from respiratory viruses. While colds and the flu are difficult to escape completely, there are effective ways to reduce their spread within your household and protect your loved ones. Here’s your go-to survival guide to navigating this season with confidence....
Shop Austin Air Systems
Discover the full line of Austin Air products and decide which one is best for your needs.
Contact
716-856-3700
Business Hours: Monday - Friday 8:30 Am To 5:00 Pm Eastern Standard Time

Copyright © 2024 AustinAir. All Rights Reserved.
Check out our socials
*Disclosure: Monthly financing through Klarna issued by WebBank. Other CA resident loans made or arranged pursuant to a California Financing Law license. NMLS # 1353190.


